Abstract
Background: Sepsis is a life-threatening condition characterized by organ dysfunction caused by a dysregulated host response to infection. Despite improvements in clinical management, both incidence and mortality remain high. Identifying biomarkers with high sensitivity and specificity is critical for early diagnosis. CD64, an Fcγ receptor upregulated on neutrophils during infection, has emerged as a promising diagnostic indicator. This study aimed to evaluate the diagnostic and mechanistic role of CD64 in pediatric sepsis.
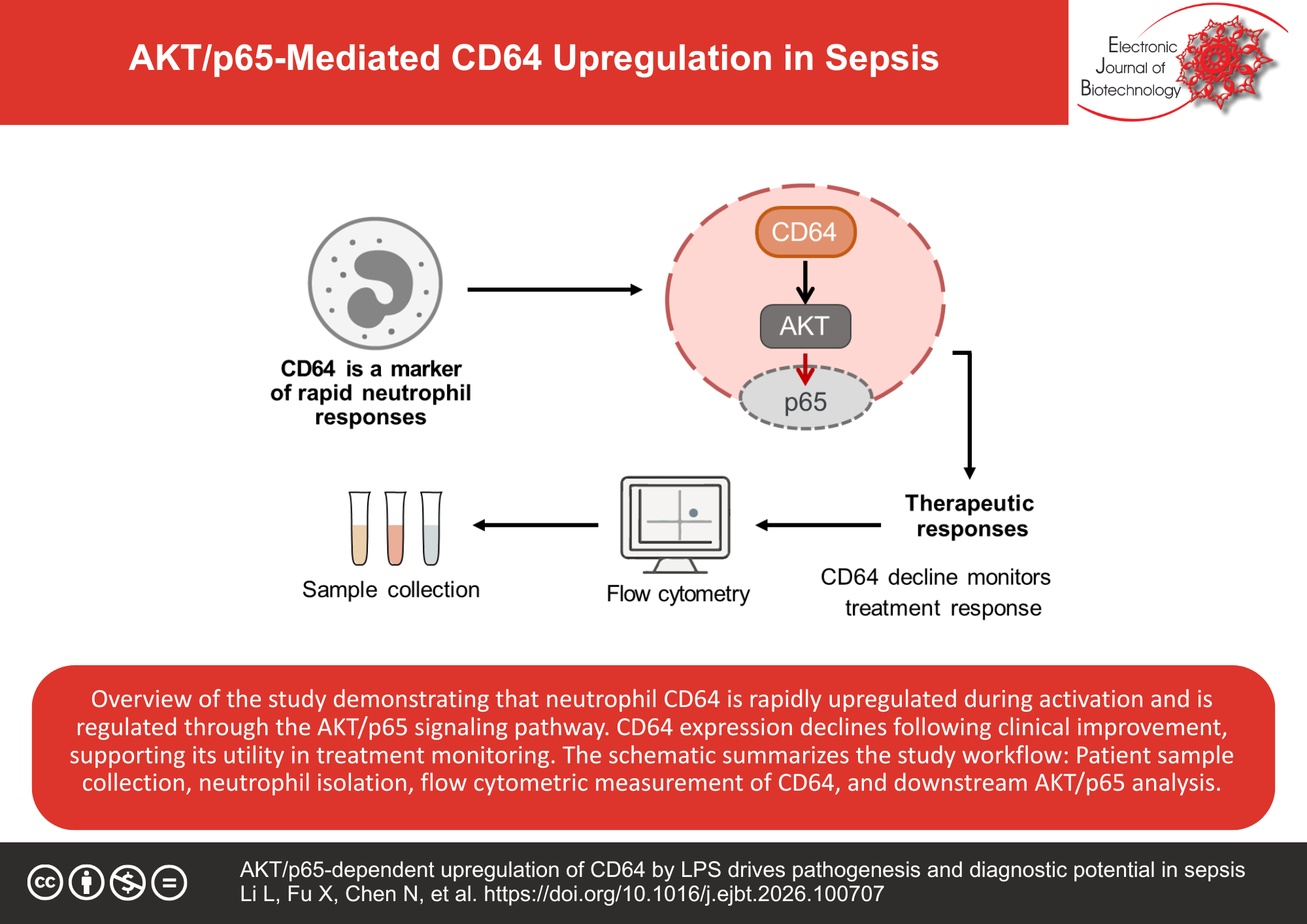
Results: A total of 200 children with sepsis and 166 healthy controls were enrolled. At a cutoff value of 0.165, the CD64 index achieved a diagnostic sensitivity of 87.0% and specificity of 92.8%, outperforming conventional markers such as procalcitonin (PCT), C-reactive protein (CRP), interleukin-1β (IL-1β), and interleukin-6 (IL-6). Mechanistic assays demonstrated that lipopolysaccharide (LPS) stimulation induced CD64 expression through the Protein Kinase B (AKT) signaling pathway. Both LPS exposure and AKT overexpression promoted p65 nuclear translocation, and chromatin immunoprecipitation confirmed p65 binding to the CD64 promoter, thereby enhancing CD64 transcription.
Conclusions: CD64 exhibits superior diagnostic and prognostic performance compared to traditional inflammatory markers and serves as a reliable biomarker for pediatric sepsis. Mechanistically, CD64 upregulation is mediated by the AKT/p65 signaling axis. These findings provide a foundation for integrating CD64 into early diagnostic workflows and developing targeted therapeutic strategies in sepsis management.
References
Balamuth F, Scott HF, Weiss SL, et al. Validation of the pediatric sequential organ failure assessment score and evaluation of Third International Consensus Definitions for Sepsis and Septic Shock Definitions in the Pediatric Emergency Department. JAMA Pediatrics 2022;176(7):672-678. https://doi.org/10.1001/jamapediatrics.2022.1301 PMid: 35575803
Singer M, Deutschman CS, Seymour CW, et al. The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3). JAMA 2016;315(8):801-810. https://doi.org/10.1001/jama.2016.0287 PMid: 26903338
Tan B, Wong JJ, Sultana R, et al. Global Case-Fatality Rates in Pediatric Severe Sepsis and Septic Shock: A Systematic Review and Meta-analysis. JAMA Pediatrics 2019;173(4):352-362. https://doi.org/10.1001/jamapediatrics.2018.4839 PMid: 30742207
Liu B, Du H, Zhang J, et al. Developing a new sepsis screening tool based on lymphocyte count, international normalized ratio and procalcitonin (LIP score). Scientific Reports 2022;12(1):20002. https://doi.org/10.1038/s41598-022-16744-9 PMid: 36411279
Yeh CF, Wu CC, Liu SH, et al. Comparison of the accuracy of neutrophil CD64, procalcitonin, and C-reactive protein for sepsis identification: A systematic review and meta-analysis. Annals of Intensive Care 2019;9:5. https://doi.org/10.1186/s13613-018-0479-2 PMid: 30623257
Hassan U, Ghonge T, Reddy B Jr, et al. A point-of-care microfluidic biochip for quantification of CD64 expression from whole blood for sepsis stratification. Nature Communications 2017;8:15949. https://doi.org/10.1038/ncomms15949 PMid: 28671185
Li S, Huang X, Chen Z, et al. Neutrophil CD64 expression as a biomarker in the early diagnosis of bacterial infection: a meta-analysis. International Journal of Infectious Diseases 2013;17(1):e12-23. https://doi.org/10.1016/j.ijid.2012.07.017 PMid: 22940278
Dal Ponte ST, Alegretti AP, Pilger DA, et al. Diagnostic accuracy of CD64 for sepsis in Emergency Department. Journal of Global Infectious Diseases 2018;10(2):42-46. https://doi.org/10.4103/jgid.jgid_91_17 PMid: 29910563
Ren Q, Guo F, Tao S, et al. Flavonoid fisetin alleviates kidney inflammation and apoptosis via inhibiting Src-mediated NF-?B p65 and MAPK signaling pathways in septic AKI mice. Biomedicine & Pharmacotherapy 2020;122:109772. https://doi.org/10.1016/j.biopha.2019.109772 PMid: 31864140
Peng W, Chen L, Liu J. Celastrol inhibits gastric cancer cell proliferation, migration, and invasion via the FOXA1/CLDN4 axis. Toxicology Research 2023;12(3):392-399. https://doi.org/10.1093/toxres/tfad024 PMid: 37397926
Liu Q, Gao Y, Yang T, et al. nCD64 index as a novel inflammatory indicator for the early prediction of prognosis in infectious and non-infectious inflammatory diseases: An observational study of febrile patients. Frontiers in Immunology 2022;13:905060. https://doi.org/10.3389/fimmu.2022.905060 PMid: 35967346
Nakagawa NK, Cruz RJ Jr, Aikawa P, et al. Pentoxifylline attenuates leukocyte-endothelial interactions in a two-hit model of shock and sepsis. Journal of Surgical Research 2015;193(1):421-428. https://doi.org/10.1016/j.jss.2014.07.034 PMid: 25224275
Hashem HE, El Masry SA, Mokhtar AM, et al. Valuable role of neutrophil CD64 and highly sensitive CRP biomarkers for diagnostic, monitoring, and prognostic evaluations of sepsis patients in neonatal ICUs. BioMed Research International 2020;2020:6214363. https://doi.org/10.1155/2020/6214363 PMid: 33204274
Dai J, Jiang W, Min Z, et al. Neutrophil CD64 as a diagnostic marker for neonatal sepsis: Meta-analysis. Advances in Clinical and Experimental Medicine 2017;26(2):327-332. https://doi.org/10.17219/acem/58782 PMid: 28791853
Weiss SL, Peters MJ, Alhazzani W, et al. Surviving sepsis campaign international guidelines for the management of septic shock and sepsis-associated organ dysfunction in children. Intensive Care Medicine 2020;46(1):10-67. https://doi.org/10.1007/s00134-019-05878-6 PMid: 31787045
Barichello T, Generoso JS, Singer M, et al. Biomarkers for sepsis: more than just fever and leukocytosis-a narrative review. Critical Care 2022;26(1):14. https://doi.org/10.1186/s13054-021-03862-5 PMid: 35026035
Patnaik R, Azim A, Agarwal V. Neutrophil CD64 a diagnostic and prognostic marker of sepsis in adult critically Ill patients: A brief review. Neutrophil CD64 in Sepsis for Diagnosis and Prognosis. Indian Journal of Critical Care Medicine 2020;24(12):1242-1250. https://doi.org/10.5005/jp-journals-10071-23558 PMid: 33568878
Li A, Ling L, Qin H, et al. Epidemiology, management, and outcomes of sepsis in ICUs among countries of differing national wealth across Asia. American Journal of Respiratory and Critical Care Medicine 2022;206(9):1107-1116. https://doi.org/10.1164/rccm.202201-0153OC PMid: 35767555
Rathinam VAK, Zhao Y, Shao F. Innate immunity to intracellular LPS. Nature Immunology 2019;20(5):527-533. https://doi.org/10.1038/s41590-019-0368-3 PMid: 30962590
Gunn JS, Ernst RK. The structure and function of Francisella lipopolysaccharide. Annals of the New York Academy of Sciences 2007;1105(1):202-218. https://doi.org/10.1196/annals.1409.006 PMid: 17395722
Stelmasiak M, Slotwinski R. Infection-induced innate antimicrobial response disorders: from signaling pathways and their modulation to selected biomarkers. Central European Journal of Immunology 2020;45(1):104-116. https://doi.org/10.5114/ceji.2020.94712 PMid: 32425688
Chen XS, Wang SH, Liu CY, et al. Losartan attenuates sepsis-induced cardiomyopathy by regulating macrophage polarization via TLR4-mediated NF-?B and MAPK signaling. Pharmacological Research 2022;185:106473. https://doi.org/10.1016/j.phrs.2022.106473 PMid: 36216272
Luan G, Pan F, Bu L, et al. Butorphanol promotes macrophage phenotypic transition to inhibit inflammatory lung injury via ? receptors. Frontiers in Immunology 2021;12:692286. https://doi.org/10.3389/fimmu.2021.692286 PMid: 34421922
Zhang F, Qi L, Feng Q, et al. HIPK2 phosphorylates HDAC3 for NF-?B acetylation to ameliorate colitis-associated colorectal carcinoma and sepsis. Proceedings of the National Academy of Sciences of the United States of America2021;118(28):e2021798118. https://doi.org/10.1073/pnas.2021798118 PMid: 34253593
Zhang H, Liu L, Li L. Lentivirus-mediated knockdown of Fc?RI (CD64) attenuated lupus nephritis via inhibition of NF-?B regulating NLRP3 inflammasome activation in MRL/lpr mice. Journal of Pharmacological Sciences 2018;137(4):342-349. https://doi.org/10.1016/j.jphs.2018.05.012 PMid: 30190171
Rasslan R, Utiyama EM, Marques GM, et al. Inflammatory activity modulation by hypertonic saline and pentoxifylline in a rat model of strangulated closed loop small bowel obstruction. Int J Surg 2014;12(6):594-600. https://doi.org/10.1016/j.ijsu.2014.04.007 PMid: 24797690
Reinhart K, Daniels R, Kissoon N, et al. Recognizing Sepsis as a Global Health Priority - A WHO Resolution. The New England Journal of Medicine 2017;377(5):414-417. https://doi.org/10.1056/NEJMp1707170 PMid: 28658587
Fleischmann-Struzek C, Goldfarb DM, Schlattmann P, et al. The global burden of paediatric and neonatal sepsis: A systematic review. The Lancet Respiratory Medicine 2018;6(3):223-230. https://doi.org/10.1016/S2213-2600(18)30063-8 PMid: 29508706
Eichberger J, Resch E, Resch B. Diagnosis of neonatal sepsis: The role of inflammatory markers. Frontiers in Pediatrics 2022;10:840288. https://doi.org/10.3389/fped.2022.840288 PMid: 35493557
Biron BM, Ayala A, Lomas-Neira JL. Biomarkers for sepsis: What is and what might be? Biomarker Insights 2015;10(Suppl 4):7-17. https://doi.org/10.4137/BMI.S29519 PMid: 25674998
Zhang JN, Ma Y, Wei XY, et al. Remifentanil protects against lipopolysaccharide-induced inflammation through PARP-1/NF-?B signaling pathway. Mediators of Inflammation 2019;2019(1):3013716. https://doi.org/10.1155/2019/3013716 PMid: 31885481
Rudensky B, Sirota G, Erlichman M, et al. Neutrophil CD64 expression as a diagnostic marker of bacterial infection in febrile children presenting to a hospital emergency department. Pediatric Emergency Care 2008;24(11):745-748. https://doi.org/10.1097/PEC.0b013e31818c2679 PMid: 18955911
Fang DH, Fan CH, Li J, et al. Ratios of CD64 expressed on neutrophils, monocytes, and lymphocytes may be a novel method for diagnosis of neonatal sepsis. The Journal of Infection in Developing Countries 2015;9(2):175-181. https://doi.org/10.3855/jidc.5458 PMid: 25699491
El Shimi MS, Abou Shady NM, Hamed GM, et al. Significance of neutrophilic CD64 as an early marker for detection of neonatal sepsis and prediction of disease outcome. The Journal of Maternal-Fetal & Neonatal Medicine 2017;30(14):1709-1714. https://doi.org/10.1080/14767058.2016.1223030 PMid: 27578316

This work is licensed under a Creative Commons Attribution-ShareAlike 4.0 International License.
Copyright (c) 2026 Electronic Journal of Biotechnology